New Colorectal Cancer Diagnoses Fall by One-Third and Colonoscopies Grind to a Halt During Height of COVID-19

Deferral of care during COVID-19 has emerged as a growing concern for healthcare professionals and public health leaders. We’ve seen the trend everywhere: emergency departments, dentists’ offices, surgery centers, and labs. With most of the country hunkered down in their homes doing their best to minimize the risk of exposure to coronavirus, many people have been avoiding hospitals and doctors’ offices at almost any cost.
But what happens when that avoidance continues for months and people with serious conditions either don’t get diagnosed or don’t get the treatment they need? That’s the big issue confronting healthcare in the wake of COVID-19 and it’s one that we’re only just beginning to quantify.
Spotlight on Colorectal Cancer
As part of our ongoing examination of the ripple effects of COVID-19 on the U.S. healthcare system, we’ve teamed with Fight Colorectal Cancer (Fight CRC), the patient advocacy group, to track the impacts of COVID-19 on a critical segment of the population: people being treated and screened for colorectal cancer.
It is important to examine colorectal cancer trends because early detection and treatment of this common and fast-moving disease can be incredibly successful in combating the illness. Colorectal cancer is the second-leading cause of cancer death in the U.S., but early screening and detection have been key to steadily improving survival rates. Between 1970 and 2016, colorectal cancer death rates declined 51%, largely due to increased screening. When colorectal cancer is found at an early stage, the five-year survival rate is roughly 90%.
As cancer patients undergo immunosuppressive treatments, COVID-19 is of particular concern. These concerns may have implications for everything from healthcare facilities’ safety measures to the mental health ramifications and support systems needed in the patient community.
What We Found
To get to the root of exactly how COVID-19 was affecting this segment of the population, we analyzed our nationwide database of real-world patient encounters to track trends in colonoscopies, biopsies, diagnoses, and colon cancer surgeries during the pandemic and compared those trends to national averages prior to the pandemic. Fight CRC also conducted a survey and focus groups with colorectal cancer patients and survivors to understand their experiences first-hand.
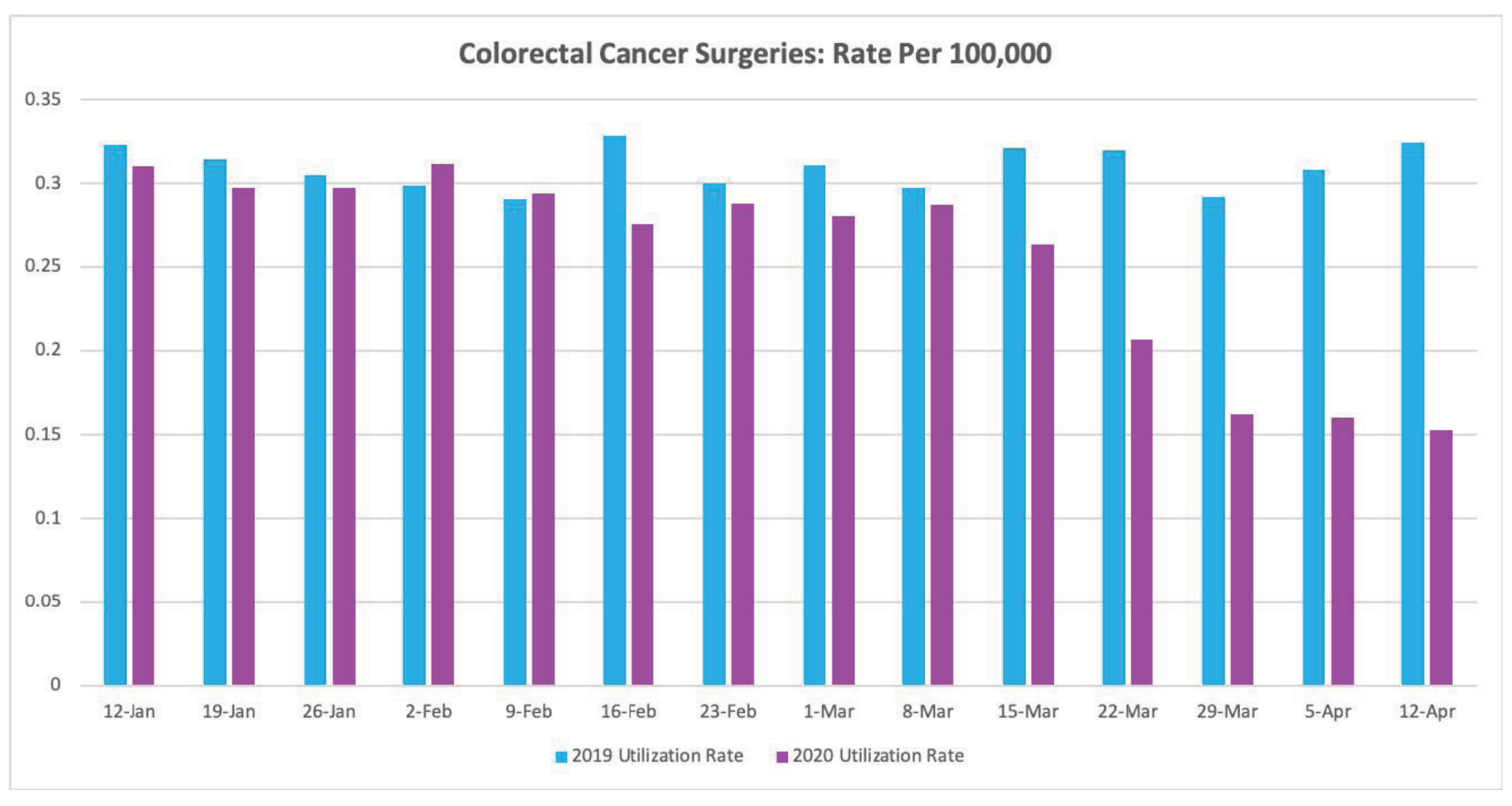
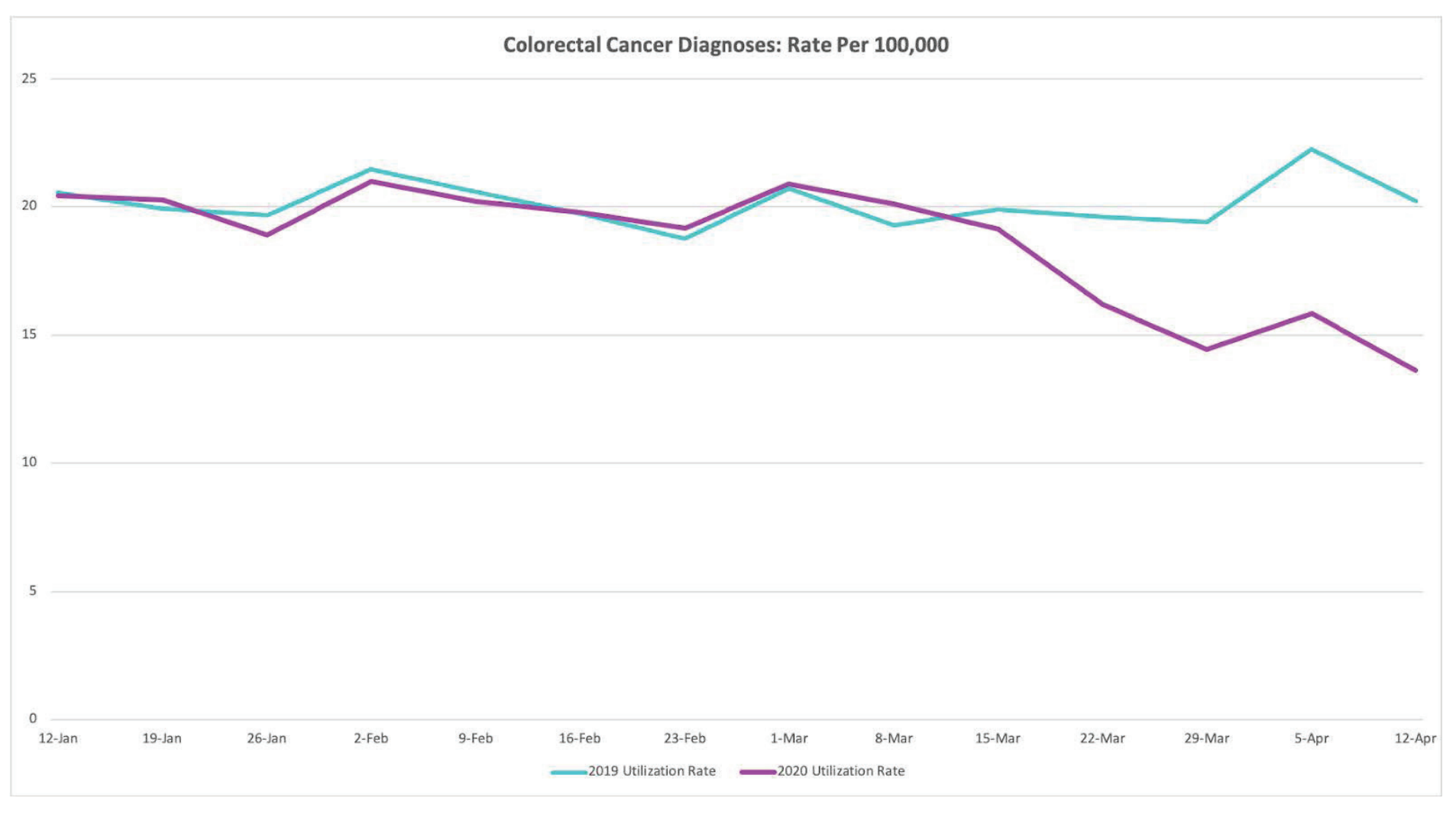
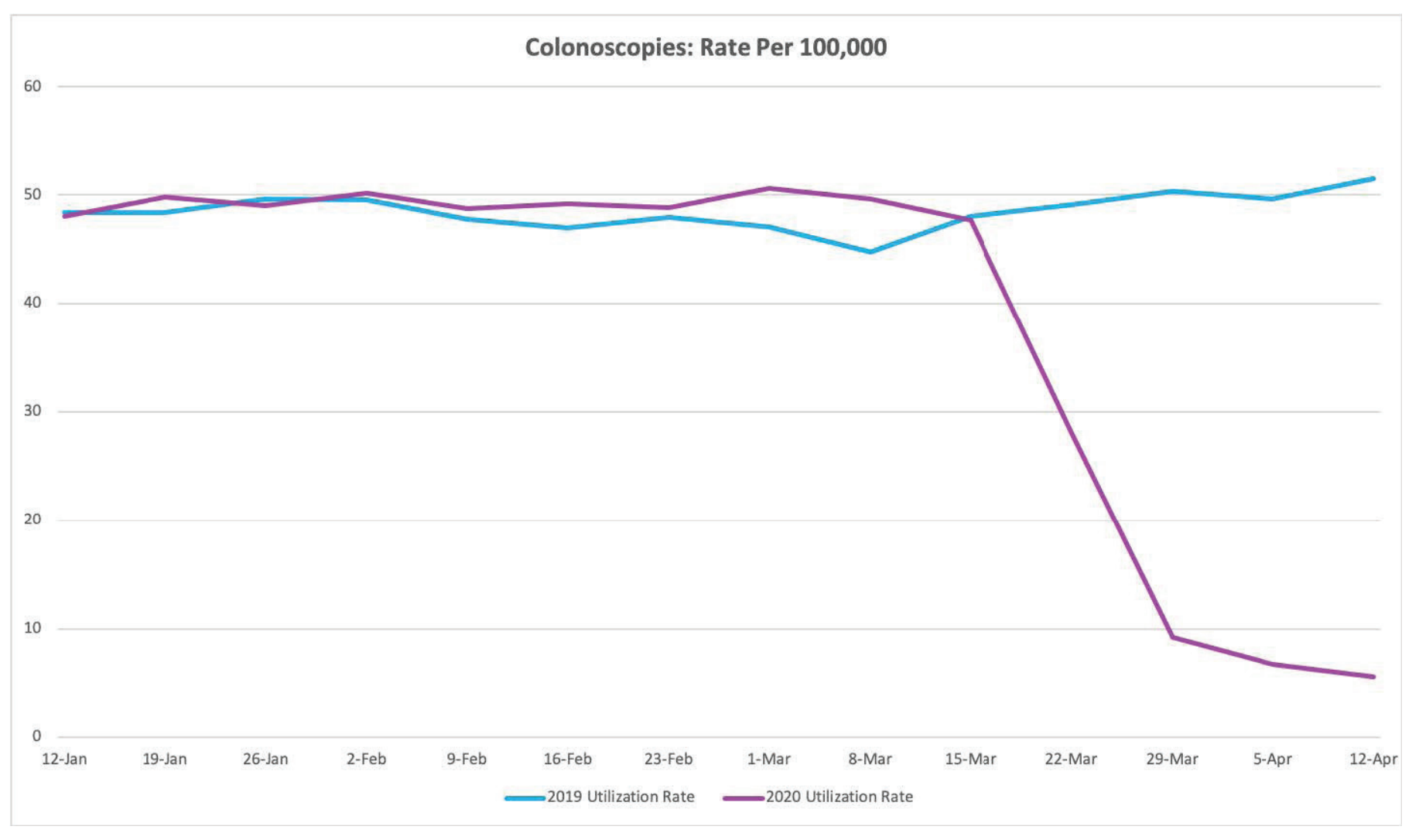
The results were stark. The total number of colonoscopies and biopsies performed declined by nearly 90% by mid-April compared to the same period last year. New colorectal cancer diagnoses were down more than 32% by mid-April, and colorectal cancer surgeries fell by 53% compared to year-ago figures.
 Nearly 40% of colorectal cancer patients and caregivers reported disruptions in their care, especially as it relates to in-person visits and imaging. Of these, 25% said they did not know when their care would be rescheduled and 34% said their visits changed to telehealth.
Nearly 40% of colorectal cancer patients and caregivers reported disruptions in their care, especially as it relates to in-person visits and imaging. Of these, 25% said they did not know when their care would be rescheduled and 34% said their visits changed to telehealth.
In addition to these clinical concerns, the pandemic has also taken a toll on the mental health of this patient community. A majority (78%) of colorectal cancer patients feel nervous, anxious, or on edge, and 57% reported they are concerned about contracting COVID-19. Twenty percent reported feelings of isolation.
Looking Ahead
These findings underscore the need for public health and health system policies that can identify and prioritize our most vulnerable populations and fast-track the process of getting them the care they need—both preventive and acute. This will be particularly important for patients actively being treated and high-risk patients with family histories of disease who simply cannot afford to delay care.
Download the research brief to learn more.