Inside the 2022 Monkeypox Outbreak

Authors: Molly Wilson, PhD, Customer Success Manager, Jack McLean, Senior Customer Success Associate, and Tabby Khan, MD, MPH, Medical Director.
After more than two years under the cloud of the COVID-19 pandemic, the world has refixed its eye on a different virus: monkeypox.
First identified in 1958, the virus that causes monkeypox had its first U.S. outbreak in 2003 when 70 cases were reported. The 2022 outbreak, which was first detected in the United Kingdom in mid-May, has, as of August 22nd, seen more than 56,000 cases in over 100 countries, with upwards of 21,000 of those cases recorded in the U.S. That has led the Biden administration to declare the monkeypox outbreak a public health emergency.
Although both COVID and monkeypox are transmissible via respiratory secretions, many monkeypox cases have stemmed from close physical contact with an infected person. Public health officials have suggested that transmission is avoidable, with WHO Director-General Tedros Adhanom Ghebreyesus advising, “This is an outbreak that can be stopped if countries, communities, and individuals inform themselves, take the risk seriously, and take the steps needed to stop transmission and protect vulnerable groups.” All the while, the world is trying to sift its way through scary headlines and make sense of yet another global health crisis.
In order to demystify the virus and understand how and where it is spreading, clear and timely data is needed. That’s why — in an attempt to decode how monkeypox has historically behaved and who it is affecting now — we have conducted a brief analysis of patients diagnosed with monkeypox in 2022. Insights are drawn from our Healthcare Map™, the industry’s largest and most complete database of de-identified, real-world patient journeys, which tracks individual encounters with the healthcare system for over 330 million patients. Our initial analysis found:
Racial, ethnic, and gender disparities already exist, but it’s not too late to change the outcomes
During the 2022 outbreak, monkeypox diagnoses have been far more predominantly male (91% male and 9% female). This imbalance supports current research that this year’s outbreak may be disproportionately impacting men who have sex with men, according to a study published in The New England Journal of Medicine. Clinicians and scientists in sexual health are engaged in a heated debate over whether monkeypox is actually a sexually transmitted infection, as monkeypox isn’t limited to spreading to certain demographics of people.
When looking at cases where race and ethnicity data are available for a patient, data suggests that monkeypox is already disproportionately impacting people of color, specifically Black Americans, who currently make up 28% of all monkeypox cases, while only comprising 14% of the total U.S. population.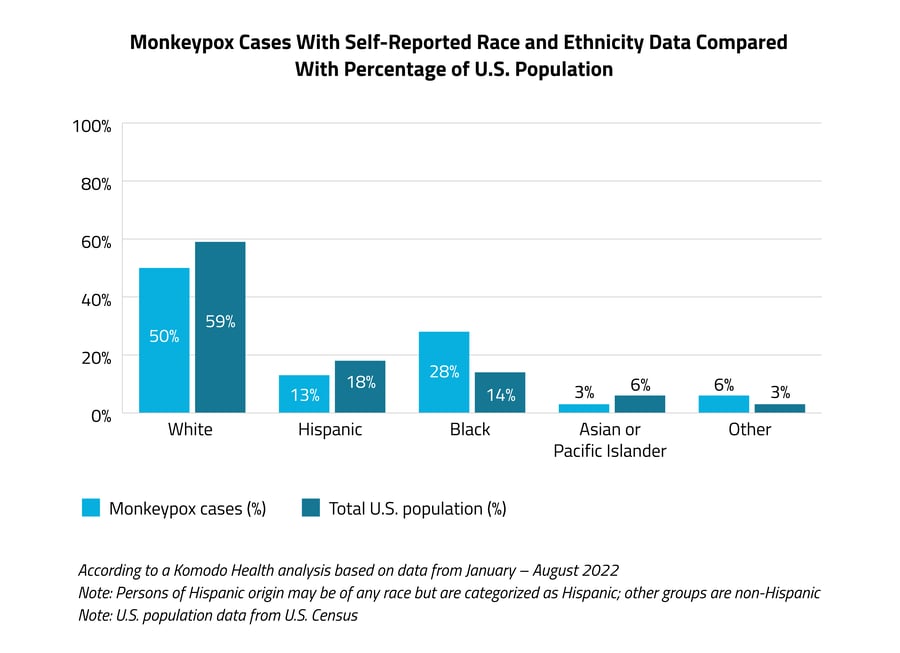
Our analysis found that the average age of a patient with monkeypox is 39. This suggests the disproportionate burden seen in the Black community is shouldered heavily by the younger population..png?width=900&name=BLOG-%20Monkeypox%20Analysis2%20(1).png) Self-reported race and ethnicity data for patients with monkeypox has been hard to come by. As of mid-August 2022, only 38% of all cases reported to the CDC had self-reported R&E data. Given our Healthcare Map’s breadth of R&E data, our analysis includes more patient information, with approximately 50% of cases having self-reported R&E information. Although complete demographic characteristics for all patients aren’t yet available, our Healthcare Map provides important additional context that helps to better understand where, how, and who is being impacted by the monkeypox outbreak. As we know from COVID-19, it is critical we analyze as much data as is available to understand the occurrence, treatment, and outcomes of this rapidly changing disease to avoid and address disparities in care.
Self-reported race and ethnicity data for patients with monkeypox has been hard to come by. As of mid-August 2022, only 38% of all cases reported to the CDC had self-reported R&E data. Given our Healthcare Map’s breadth of R&E data, our analysis includes more patient information, with approximately 50% of cases having self-reported R&E information. Although complete demographic characteristics for all patients aren’t yet available, our Healthcare Map provides important additional context that helps to better understand where, how, and who is being impacted by the monkeypox outbreak. As we know from COVID-19, it is critical we analyze as much data as is available to understand the occurrence, treatment, and outcomes of this rapidly changing disease to avoid and address disparities in care.
Widespread provider education is critical to combat spread and reduce transmission
Primary care physicians (PCPs) have most frequently diagnosed monkeypox cases this year (31%), followed by infectious disease doctors (23%), and emergency practitioners (15%). The most common symptoms presented at the time of diagnosis were rash and non-specific skin eruption (13%), other specified diseases of the anus and rectum (6%), and fever (6%). With the majority of cases being diagnosed by PCPs with non-specific symptoms, it’s more important than ever that provider education programs are comprehensive and widespread to ensure that those who are seeing patients are able to quickly identify symptoms, accurately diagnose, and effectively treat the disease. A comprehensive PCP outreach and education program also includes ensuring patients understand how to avoid spreading the disease to others.
The disease may be spreading, but so is effective treatment
During the 2022 outbreak, 59% of patients diagnosed with monkeypox only had one clinical visit related to the disease. The number of patients who were seen more than once after their initial diagnosis is even lower (41%), suggesting that monkeypox patients are not taxing an already overburdened healthcare system with additional complications from their disease.
While the data seems encouraging and ultimately should alleviate the broader population’s concerns, it comes with the caveat that the situation is fluid and evolving. But if we have learned anything since 2020, it’s that the more exhaustive the data, the better public health practitioners and patients can understand risk and make informed choices about their healthcare. Analyses like these ultimately helps inform policymakers on where to focus their efforts, and what recommendations they can make to reduce the burden of disease.
For more research about how pandemics impact health outcomes, read “How the Pandemic Has Set Back HIV Prevention, Screening and Diagnosis.”
To see more articles like this, follow Komodo Health on Twitter, LinkedIn, or YouTube, and visit Insights on our website.







