How the Pandemic Has Set Back HIV Prevention, Screening, and Diagnosis

Authors: Reyn Kenyon, MS, Customer Success Manager, Kristina Cheng, Data Scientist, Gabriel Roybal-Jungemann, PhD, Director of Customer Success, Tabby Khan, MD, MPH, Medical Director, and Alex Enrique, Healthcare Data Analyst.
Human immunodeficiency virus (HIV) and acquired immunodeficiency syndrome (AIDS) spread across the globe in the1980s and early 1990s, with a particularly devastating impact on the LGBTQ+ community. According to the World Health Organization, by the end of 2020, nearly 80 million individuals worldwide had been infected, and over 36 million had died of HIV/AIDS.
Although there is no cure for HIV, medical advances over the past decade have made it possible for HIV-positive patients to live longer and healthier lives than ever before. Like many chronic diseases, prevention, screenings, early diagnosis, and timely intervention are critical to minimize negative outcomes. For at-risk individuals, a daily dose of pre-exposure prophylaxis (PrEP) medication, such as Truvada or Descovy, markedly reduces the chances of contracting HIV. For most HIV-positive patients, antiretroviral therapies suppress viral loads to undetectable levels within six months of starting treatment, preventing further progression and minimizing transmission of the disease.
This Pride Month, DragonPride, Komodo’s affinity group for the LGBTQIA+ community and allies, investigated the impact of the COVID-19 pandemic on the prevention, screening, and diagnosis of HIV across racial and ethnic groups.
We compared counts of HIV screenings, new HIV diagnoses, new PrEP prescriptions, and PrEP adherence between the periods of March 2019 to March 2020 (pre-pandemic) and March 2020 to March 2021 (during the pandemic). We then segmented this analysis by race to determine if the pandemic differentially impacted communities of color, and looked at the locations of treatment centers to understand where patients were being seen.
Rates of HIV prevention, screening, and diagnosis declined during the pandemic.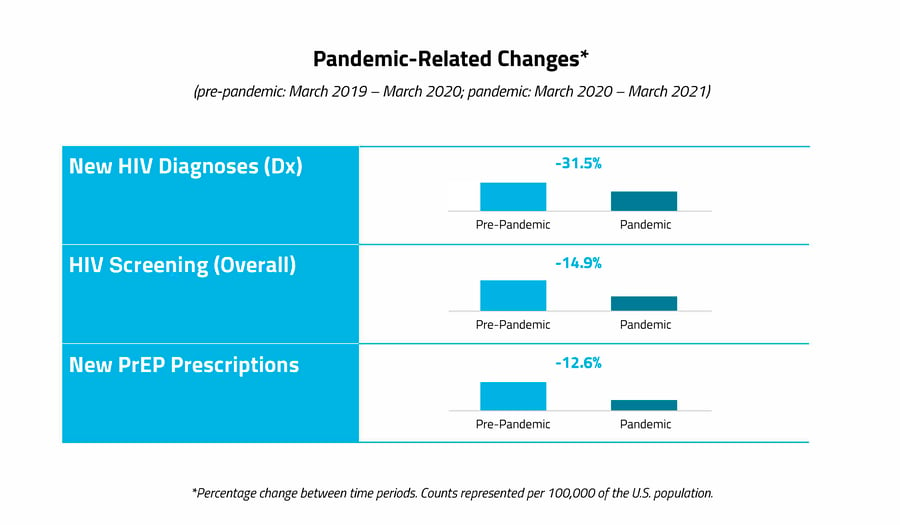 Similar to trends we’ve seen in other therapeutic areas during the pandemic, new PrEP prescriptions dropped by almost 13%, HIV screening dropped by nearly 15%, and new HIV diagnoses dropped by almost 32% among all groups in the year following the onset of the pandemic.
Similar to trends we’ve seen in other therapeutic areas during the pandemic, new PrEP prescriptions dropped by almost 13%, HIV screening dropped by nearly 15%, and new HIV diagnoses dropped by almost 32% among all groups in the year following the onset of the pandemic.
Significant racial disparities in HIV screening and diagnosis existed before and continued during the pandemic.
The Black population made up 34% of patients who were screened and 45% of all new HIV diagnoses during the period before the pandemic. This far exceeds the proportion of the American population identified as Black, which is roughly 13%. These disparities persisted throughout the pandemic, when Black Americans accounted for 44% of new diagnoses but only 35% of tests. Because screening is essential to curb the spread of a virus, these findings highlight the need for increased efforts to ensure equitable access to screening.
There were race-based gaps in PrEP adherence both before and during the pandemic.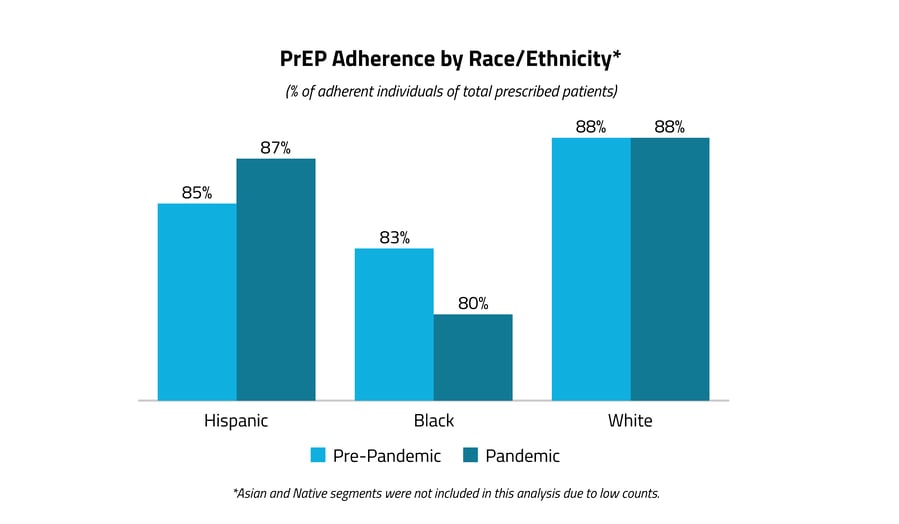
In this analysis, PrEP adherence was defined as refilling an existing PrEP prescription within 90 days of finishing the previous supply. PrEP adherence was lower in the Black population than in Hispanic and White populations, both before (83%) and during (80%) the pandemic. The Black population was the only group to experience a drop in PrEP adherence, suggesting there were significant racial disparities prior to the pandemic, which may be related to issues of equitable access to prescribed medications. Because our analysis is limited primarily to insights from commercial insurance claims and does not account for care delivered in free clinics, the actual gap could be even more severe.
Community centers are vital points of care for HIV prevention.
Community centers were the primary source of new PrEP prescriptions for all groups before the pandemic (75% of new PrEP prescriptions overall came from community vs. academic organizations) and became even more vital during the pandemic (77% of prescriptions). This trend held true across racial and ethnic groups, highlighting the fact that community organizations are key drivers of PrEP prescriptions across demographics.
While this analysis did not control for the possible impact of stay-at-home orders on sexually transmitted disease rates overall, these findings emphasize the urgent need for targeted action in communities of color to promote HIV screening and to improve access and adherence to preventive measures. To minimize any potential long-term impacts of delays in care, outreach initiatives (including public health programs and strategies that target the entire matrix of caregivers) should be undertaken to increase access to preventive healthcare. Further analyses are needed to identify and address the socioeconomic factors impacting racial disparities in PrEP adherence and to bridge the gap in HIV prevention protocols for queer Americans of color.
The disparities identified in this analysis fit with well-established trends — once again highlighting the disproportionate burden that communities of color face when navigating healthcare in America. Similar findings were identified in chronic kidney disease, colorectal cancer, and heart attack and stroke during the COVID-19 pandemic, bringing into stark clarity the need for a recalibration of the systemic, structural racism that pervades our healthcare system. It is our hope that by publishing insights such as these, we can expose the racial and ethnic disparities that persist in healthcare, close those gaps, and reduce the burden of disease.
Read more Komodo insights on the pandemic’s impact  .
.
To see more articles like this, follow Komodo Health on Twitter, LinkedIn or YouTube, and visit Insights on our website.





