Race-Based Disparities in Asthma: A Post-Pandemic Snapshot

Greater disease severity and emergency department utilization persists in cities where a higher proportion of residents are Black.
Asthma is one of the most common chronic diseases in the U.S., affecting nearly 26 million people. While most people with asthma have mild disease, it can be debilitating and even deadly, killing roughly 3,500 people in the U.S. each year. The burden of asthma falls disproportionately on some communities more than others, with higher rates of disease severity seen in Black, Hispanic, and North American Native populations as well as those in low-income communities.
The COVID-19 pandemic brought a surprising period of relief for many asthma sufferers. Asthma attacks declined, and some patients reported breathing more easily. In May 2021, we published a research brief in collaboration with the Asthma & Allergy Foundation of America that measured the impact of COVID-19 lockdowns on race-based disparities in asthma-related emergency department (ED) visits. We found that, while overall numbers of ED utilization declined, race-based gaps grew. Patients living in cities with the highest proportions of Black residents were significantly more likely to have visited an ED with an asthma-related illness than patients in cities with the lowest proportions of Black residents. The differences were stark: In New Orleans, for example, a city that is roughly 60% Black, about 1 in 3 residents with asthma visited the ED for a related condition at least once in 2020, compared to only about 1 in 10 in Salt Lake City, where only 3% of the population is Black.
We wanted to understand how race-based disparities in asthma have changed since the COVID-19 pandemic. Looking at cities with the highest and lowest proportions of Black residents in 2022, we used ICD-10-CM codes to identify patients with severe asthma, with asthma and one or more ED visits, and with asthma and a prescription for a quick-relief steroid medication. We then stratified by zip code, grouping cities with a >40% Black population and a <10% Black population, according to U.S. census data.
Here’s what we found:
Asthma patients in cities with the highest proportions of Black residents were only slightly more likely to have severe asthma compared to those in cities with the lowest proportions of Black residents.
In the cities with the six highest proportions of Black residents (Atlanta, Cleveland, Detroit, Memphis, New Orleans, and Washington, D.C.), 3.1% of asthma patients had severe asthma. This compares with 2.7% of asthma patients in cities with the lowest proportions of Black residents (Austin, Phoenix, Portland, OR, Salt Lake City, San Diego, and Seattle).
In 2022, roughly half of New Orleans residents with asthma visited the ED for an asthma-related illness.
Overall, asthma patients living in cities with the highest proportions of Black residents were 9% more likely to visit the ED in 2022 than those in cities with the lowest proportions (40% vs. 31%). Of the cities included in this analysis, the highest rate of ED visits was seen in New Orleans, which is 60% Black — 49% of asthma patients visited the ED for a related illness in 2022. The lowest rate, 25%, was seen in Portland, which is 6% Black. While asthma severity was only slightly different across groups, the much larger difference in ED visits may reflect social and structural determinants of health that can lead to an overreliance on emergency care, such as differences in insurance and access to primary and specialty care and prescribed medications.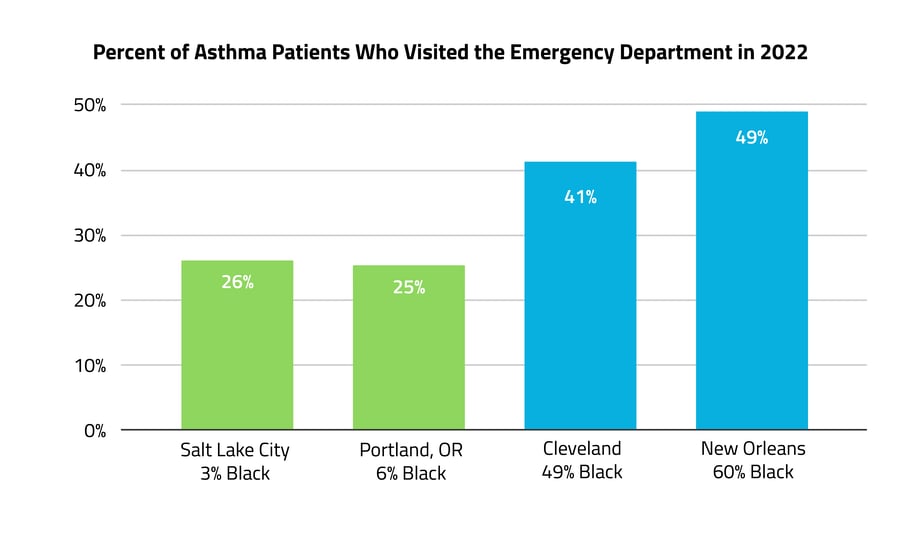 The prescription rate for quick-relief drugs (both steroidal and nonsteroidal) was 6% higher in cities with the highest proportions of Black residents compared with cities with the lowest proportions.
The prescription rate for quick-relief drugs (both steroidal and nonsteroidal) was 6% higher in cities with the highest proportions of Black residents compared with cities with the lowest proportions.
In 2022, 68% of asthma patients in cities with the highest proportion of Black residents had been prescribed a quick-relief drug. In cities with the lowest proportions, 62% of asthma patients received prescription medications.
A slightly greater difference was seen in rates of asthma patients prescribed steroidal drugs (7% higher), compared with non-steroidal drugs (5% higher). Steroidal medicines may be prescribed to treat asthma attacks when a patient hasn’t responded to other asthma medicines. Higher steroidal medicine use may indicate more severe or poorly controlled asthma.
Racial and ethnic disparities exist across most areas of health and healthcare and, as in the case of asthma, are driven by socioeconomic and environmental inequities. Disparities in asthma are intensified by the cumulative risk from these overlapping inequities.
The COVID-19 pandemic highlighted the stark inequities that exist in the U.S. healthcare system. Health equity continues to be a focus post-pandemic, and data-driven evidence is key as we move to elucidate population-wide health disparities and inform and advocate for policy changes that address race- and ethnicity-based gaps in exposure, health, and care. This evidence is particularly important for asthma, where disparities persist despite general improvement in asthma-related health outcomes over the past two decades. Population-based studies are critical to the development of public health initiatives for improving asthma outcomes.
To see more articles like this, follow Komodo Health on Twitter, LinkedIn, or YouTube, and visit Insights on our website.







