Let the Data Do the Work: MedTech Companies Reap the Value of Claims-Based Insights

The MedTech industry has a proven, three-pronged strategy for driving commercial success: Manually comb through data to understand the market, build a strong network to glean word-of-mouth intelligence, and forge deep relationships with providers to ensure needs are met.
It’s a formula that has brought commercial teams far, but its weaknesses are well known:
- Obtaining market intelligence is primarily a manual activity and thus incredibly time intensive
- Field representatives, who are already expected to excel as clinical experts and provider liaisons, must also serve as investigative sleuths
- Piecemeal information leads to patchwork roadmaps: Teams “don’t know what they don’t know,” which leads to an inefficient engagement strategy where patient journeys are misunderstood and key providers are often overlooked
Fortunately, real-world data and user-friendly technology now make it possible for MedTech companies to overcome these weaknesses and gain patient- and provider-level insights faster and more efficiently. With access to innovative capabilities such as predictive analytics, and to demographic data such as race and ethnicity, teams are able to see and do things they’ve never done before.
Playing Catch Up
While some MedTech companies are already on the bandwagon, the industry as a whole is lagging behind Pharma, and there appear to be several reasons why. At a recent Komodo-sponsored webinar, attendees shared multiple concerns with using claims-based data as their primary source of market intelligence. 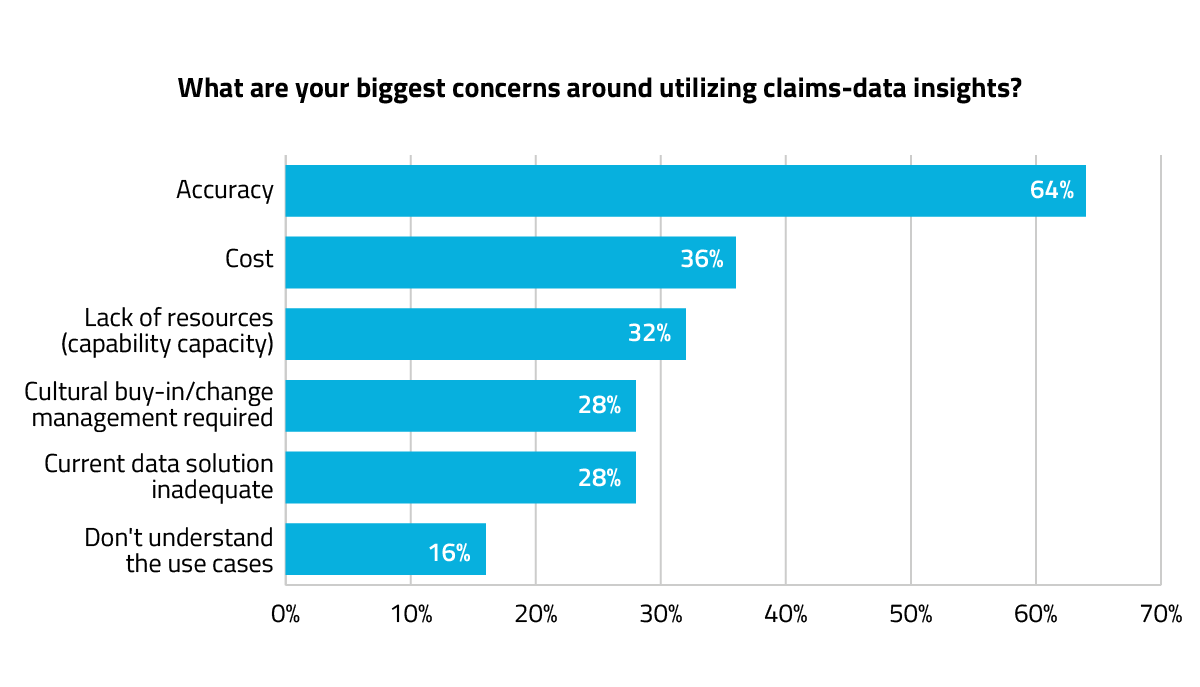 By far, data accuracy was cited as the greatest concern. This skepticism isn’t unusual and is, in fact, wise. Understanding how patient-level data is sourced, linked, and deduplicated is crucial to ensuring it’s trustworthy. Moreover, teams should scrutinize what open- vs. closed-claims data can reveal, as the former delivers only a snapshot in time, which can skew inferences, while the latter captures all clinical interactions. Understanding in advance what insights are possible enables teams to compare their current time and cost investments with what data + SaaS brings to the table. This includes not only getting a grasp on data accuracy, but also on the speed and granularity — or “richness” — of insights and how those might accelerate and increase commercial success.
By far, data accuracy was cited as the greatest concern. This skepticism isn’t unusual and is, in fact, wise. Understanding how patient-level data is sourced, linked, and deduplicated is crucial to ensuring it’s trustworthy. Moreover, teams should scrutinize what open- vs. closed-claims data can reveal, as the former delivers only a snapshot in time, which can skew inferences, while the latter captures all clinical interactions. Understanding in advance what insights are possible enables teams to compare their current time and cost investments with what data + SaaS brings to the table. This includes not only getting a grasp on data accuracy, but also on the speed and granularity — or “richness” — of insights and how those might accelerate and increase commercial success.
Seeing is Believing
MedTech companies who have embraced using tech-generated insights are already seeing the payoff. In the November webinar, Iterative Health’s Director of Sales, Neal Smith, shared the challenges of identifying gastroenterologists specializing in inflammatory bowel disorder (IBD) who are also involved in clinical research. He explained how his organization leverages closed-claims data to find these providers with pinpoint accuracy, faster.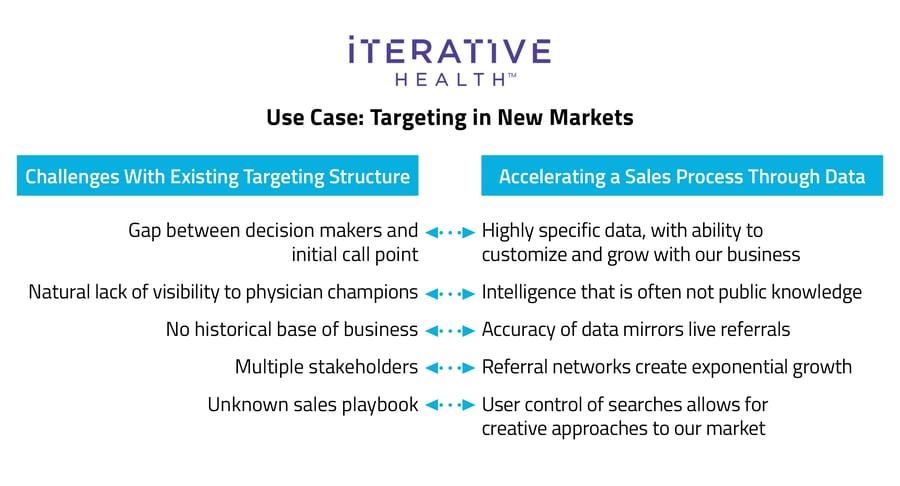 “I can say that the specificity and accuracy of the data has been one of the most empowering aspects,” said Smith. “We're able to get to those doctors much more quickly than either looking online through public information, i.e., the website, or investigating with our current customers or relationships.”
“I can say that the specificity and accuracy of the data has been one of the most empowering aspects,” said Smith. “We're able to get to those doctors much more quickly than either looking online through public information, i.e., the website, or investigating with our current customers or relationships.”
Smith also shared how granular insights on referral patterns are enabling his team to reduce health disparities. “We can see where an IBD specialist who does clinical research is getting their referrals from, and in turn pursue those referring facilities that don’t offer that level of expertise to help them improve the level of care.”
Likewise, DePuy Synthes’ Kyana Stewart, U.S. Commercial Director of Innovation and Strategy for ASCs, shared how insights gained from combining internal and third-party data is helping her company with strategy and efficiency.
“As much as we rely on our field teams, the reality is they can't be everything to everybody at all times while maintaining their high level of clinical expertise,” said Stewart, “We combine internal and third-party data to gain insights that help them prioritize their bandwidth and focus on where they can have the most impact.”
Stewart said using data to reduce health disparities is a key focus for her organization as well.
“We’ve begun to think past what we believe to be true and to leverage data. We've got zip code information, commercial claims data, Medicare claims data, and site-of-care data, and then internally, we've been looking at the disparity deciles for certain disease states. Now we’re asking the question, ‘What if we could envision a state where we could leverage data to target areas of greatest need, where there's a high disparity index, and then start to craft an intervention aimed at targeting educational efforts and bringing more of those patients into sites of care to improve health equity overall?’”
Transitioning from Piecemeal to Data Driven
MedTech companies have proven themselves to be resourceful in reaching patients to improve and save lives. With real-world data and purpose-built software that surfaces volume by physician, care setting, case and payer mix, readmission/re-op rates, and patient-level R&E insights, it’s now possible to automate much of the manual work and more importantly, to obtain a more granular, highly accurate view of the patient journey, both longitudinally and in real time. In turn, these companies will no doubt forge a whole new level of success as they develop strategies to address health disparities, become more time- and cost-efficient in HCP targeting, and reach more patients, faster, to improve lives.
Learn how Komodo helps MedTech companies accelerate and increase commercial success.
Author Bio: Stephanie Eitel worked in medical device marketing for more than two decades before joining Komodo Health. She is passionate about leveraging real-world data to reach patients faster, improving their quality of life and lifespan. Stephanie received her MBA from the University of Massachusetts and her BS in Business Marketing from Colorado State University.
To see more articles like this, follow Komodo Health on Twitter, LinkedIn, or YouTube, and visit Insights on our website.







