A Shadow Pandemic: “Missing” Child Abuse Victims Slipping Through the Cracks

In the first months of the COVID-19 pandemic, United Nations Women launched the Shadow Pandemic campaign to bring attention to domestic violence intensifying as a result of health and economic stresses, cramped living conditions, and isolation.
Over the spring of 2020, as lockdowns were implemented around the world, data showed increases in internet searches related to abuse and increased call volume to domestic abuse hotlines.
As a foster parent myself, I’ve witnessed first-hand the horrific impact of domestic violence on children that I considered part of my own family. The immediate effects are gut-wrenching — and the effects of abuse ripple out well beyond a child’s early years. According to the American Society for the Positive Care of Children, children who are neglected have a 43% higher risk of dying early in adulthood and are approximately 9 times more likely to become involved in criminal activity. In addition, 14% of men and 36% of women in the U.S. prison system were abused as children, about twice the frequency seen in the general population.
The pandemic has taken away many of the safeguards in place for protecting at-risk children. Across the United States, wellness checks are required for children under 5, which provide regular opportunities for pediatricians to detect abuse. However, over the past two years, with in-person physicals and other routine check-ups deferred, and with inconsistent access to in-person learning and teachers, school nurses, and other school faculty, we hypothesized thousands of abused children may have slipped through the cracks.
With this in mind, I partnered with our Clinical Innovations team to better understand how the pandemic has impacted child abuse. Leveraging the Komodo Healthcare Map, we examined trends before and during COVID to see how children coded with abuse move through the healthcare system in the year following their diagnosis.
To define the population, we looked at three different types of abuse with the most reliable coding: neglect or abandonment, physical abuse, and unspecified maltreatment in patients, and segmented that population by the ages of 0-5 and 6-18.
Abuse Lays The Groundwork for Future Mental Health Struggles
Not surprisingly, the impacts of child abuse ripple out well beyond a child’s early years. We examined pre-COVID trends to see how children coded with abuse move through the healthcare system in the year post-diagnosis.
Among abused children from 2018-2020, we found:
- The percentage of children diagnosed with PTSD increased 109%, from 8.6% to 18.1%
- The percentage of children with anxiety increased 58%, from 7.0% to 11.1%
- The percentage of children with depression increased 45%, from 7.6% to 11.0%
While these insights likely underestimate the true numbers of psychiatric disorders, they do suggest that a child abuse diagnosis may be an important catalyst for addressing mental health challenges.
Children Slipping Through Pandemic-Created Cracks
These findings underscore the importance of identifying these children as soon as possible, not only to address physical safety needs, but also to provide critical mental health support.
Alarmingly, our analysis of child abuse trends during COVID indicates a massive problem with unreported or undetected instances of child abuse. Diagnoses dropped dramatically in the spring of 2020: In March 2020, diagnoses for those under 5 dropped 30% and diagnoses for ages 6-18 dropped by more than 40%, relative to a 2019 pre-pandemic baseline.
Diagnoses for those under 5 briefly returned to that baseline in fall 2020, but largely, diagnoses have stayed well under the baseline and, in fact, have trended downward since winter 2021. This suggests a significant population of “missing” children living in abusive situations without help or support — and the data hasn’t yet indicated a significant catch-up period to make up for the downward trends. 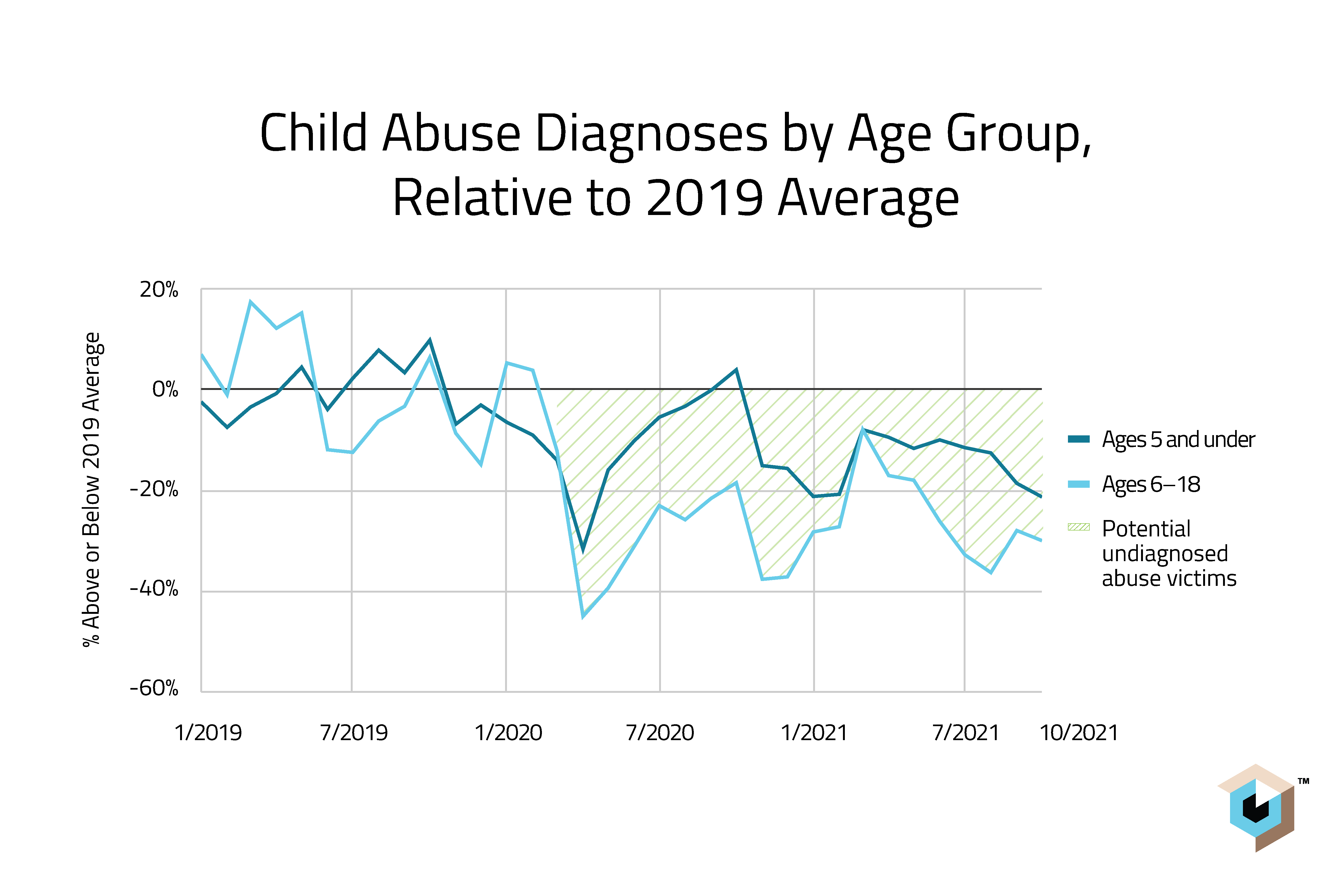 From the data, we can see that COVID has had a massive impact on child abuse diagnoses. School nurses, teachers, and other adults with whom children interact play an important role in identifying and escalating concerns about abuse. Without regular in-person interactions with these trained professionals, we may be missing key early indicators of child abuse.
From the data, we can see that COVID has had a massive impact on child abuse diagnoses. School nurses, teachers, and other adults with whom children interact play an important role in identifying and escalating concerns about abuse. Without regular in-person interactions with these trained professionals, we may be missing key early indicators of child abuse.
There may be an important opportunity for health professionals to step in and close the gap.
The Journey to Diagnosis and Opportunities for HCPs
With this in mind, we also looked at the journeys of these children through the healthcare system, and which types of doctors were most likely to flag suspected or confirmed abuse. Unsurprisingly, pediatrics and behavioral care led with 30% of diagnoses, with an especially high rate of confirmed abuse diagnoses.
But notably, 19% of child abuse diagnoses were made by emergency medicine doctors, who may see some of the first obvious signs of abuse. In the 12 months prior to a child abuse diagnosis, nearly 50% of patients went to the ER or were hospitalized. Many of these patients visited multiple times and sometimes with evidence of bruising, bone fracture, or lacerations.
While there are many reasons children visit the ER, it is also possible that indications of child abuse are present in the healthcare system well before being officially flagged and monitored.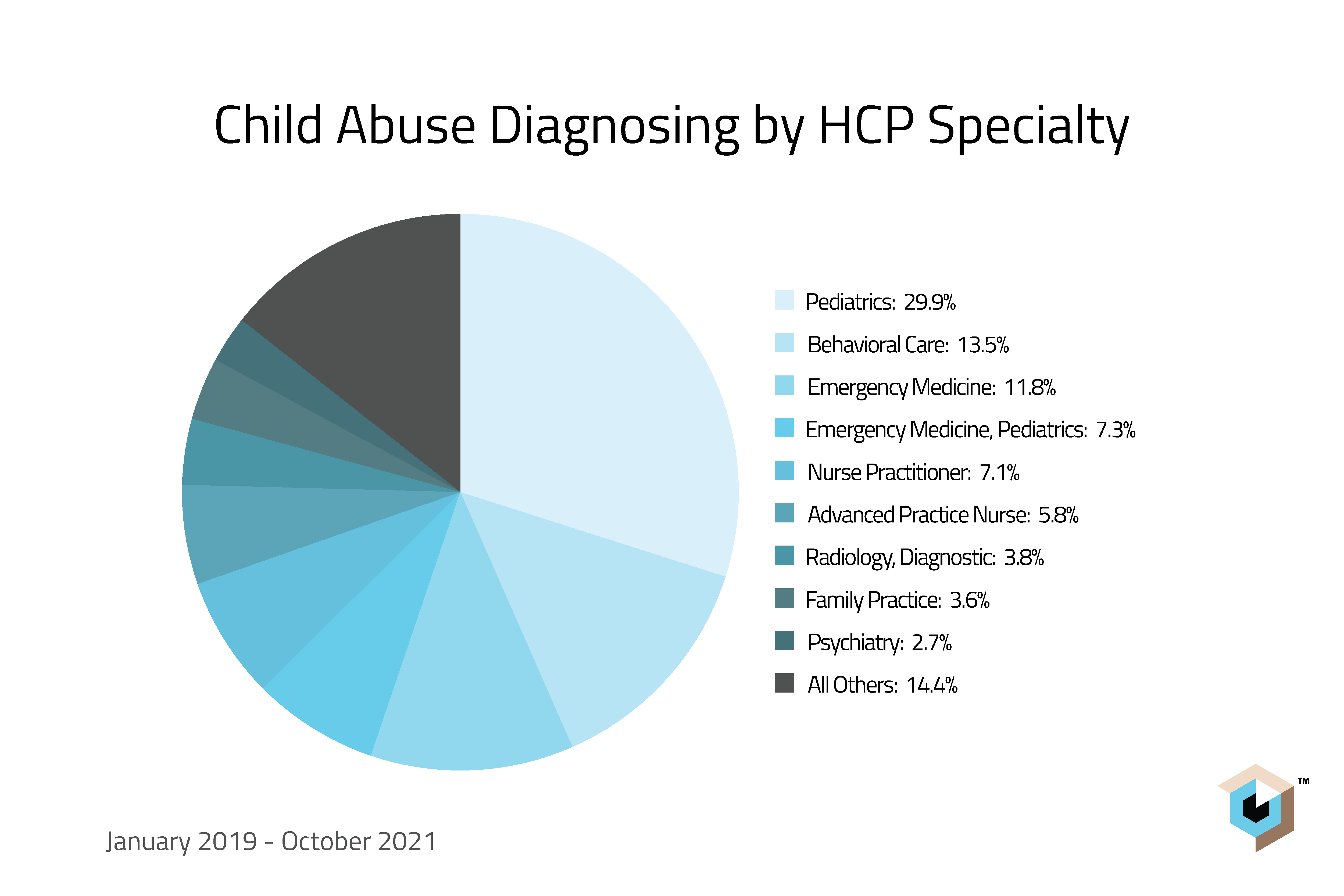 The healthcare system is only one piece of the complex puzzle of child abuse prevention, identifying at-risk children, and removing victims from dangerous situations. But these insights from the Healthcare Map provide a critical lens into how the pandemic has kept many of these children hidden from view — and the emerging role the healthcare system can play in finding these “missing” children and driving better lifetime outcomes for each of them.
The healthcare system is only one piece of the complex puzzle of child abuse prevention, identifying at-risk children, and removing victims from dangerous situations. But these insights from the Healthcare Map provide a critical lens into how the pandemic has kept many of these children hidden from view — and the emerging role the healthcare system can play in finding these “missing” children and driving better lifetime outcomes for each of them.
For more on the pandemic’s impact on healthcare outcomes,  — and diagnoses — during 2020.
— and diagnoses — during 2020.
To see more articles like this, follow Komodo Health on Twitter, LinkedIn, or YouTube, and visit Insights on our website.







